Abstract
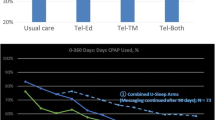
The objective of this study was to compare continuous positive airway pressure (CPAP) use, functional status, and client satisfaction in obstructive sleep apnea syndrome (OSAS) patients randomized to either telemedicine support or traditional care. In our university-affiliated sleep disorders center, patients with OSAS who were initiating CPAP therapy were randomized to receive telemedicine support vs traditional follow-up care for 30 days. The telemedicine group received a “Health Buddy” computer that provided daily Internet-based informational support and feedback for problems experienced with CPAP use. At 30 days, there were no significant differences in the hours of CPAP use between groups receiving traditional care (M=4.22, SD±2.05) and telemedicine support (M=4.29, SD±2.15), p=0.87, or in the proportion of nights with CPAP use between the traditional (M=50%±33.8) and telemedicine groups (M=47%±34.2), p=0.61. No significant differences were found between groups in functional status (M=2.27±4.56 vs M=2.03±3.88, respectively, p=0.76) or client satisfaction (M=28.0±3.51 vs M=28.5±3.05, p=0.43). Patients in the telemedicine and traditional groups had similar CPAP use, functional status, and client satisfaction. The data suggest that telemedicine support as provided by our model compares favorably with traditional care. As a provider-extender, telemedicine support for patients initiating use of CPAP may allow for greater practice efficiency while maintaining quality of care.
Similar content being viewed by others

References
Chokroverty S (1999) Sleep disorders medicine, 2nd edn. Butterworth Heinemann, Woburn, MA
National Heart (1996) Lung and blood institute working group on sleep apnea. Sleep apnea: is your patient at risk? Am Fam Physician 53:247–253
Russo-Magno P, O’Brien A, Panciera T, Rounds S (1998) Compliance with CPAP therapy in older men with obstructive sleep apnea. J Am Geriatr Soc 49:1205–1211
Chervin RD, Theut S, Bassetti C, Aldrich MS (1997) Compliance with nasal CPAP can be improved by simple interventions. Sleep 20:284–289
Hoy CJ, Vennelle M, Kingshott RN, Engleman HM, Douglas NJ (1999) Can intensive support improve continuous positive airway pressure use in patients with the sleep apnea/hypopnea syndrome? Am J Respir Crit Care Med 159:1096–1100
Likar LL, Panciera TM, Erickson AD, Rounds S (1997) Group education sessions and compliance with nasal CPAP therapy. Chest 111:1273–1277
Institute of Medicine (1996) Telemedicine: a guide to assessing telecommunications in health care. National Academy, Washington, DC
Montani S, Bellazzi R, Larizza C, Riva A, D’Annunzio G, Fiocchi S, Lorini R, Stefanelli M (1999) Protocol-based reasoning in diabetic patient management. Int J Med Inform 52:61–77
Mease A, Whitlock W, Brown A, Moore K, Pavliscsak H, Dingbaum A (2000) Telemedicine improved diabetic management. Mil Med 165:579–584
Morlion B, Verbandt Y, Paiva M, Estenne M, Michils A, Sandron P, Bawin C (1999) A telemanagement system for follow-up of respiratory patients. Eng Med Biol Mag 18:71–79
Kinne G, Droste C, Fahrenberg J, Roskamm H (1999) Symptomatic myocardial ischemia and everyday life: implications for clinical use of interactive monitoring. J Psychosom Res 46:362–377
Weaver TE, Laizner AM, Evans LK et al (1997) An instrument to measure functional status outcomes for disorders of excessive sleepiness. Sleep 20:835–843
Larsen DL, Attkisson CC, Hargeaves WA, Nguyen TD (1979) Assessment of client/patient satisfaction: development of a general scale. Eval Program Plann 2:197–207
DeMolles DA, Sparrow D, Gottlieb DJ, Friedman R (2004) A pilot trial of a telecommunications system in sleep apnea management. Med Care 42:764–769
Hui DS, Chan JK, Choy DK, Ko FW, Li TS, Leung RC, Lai CK (2000) Effects of augmented continuous positive airway pressure education and support on compliance and outcome in a Chinese population. Chest 117:1410–1416
Naegele B, Thouvard V, Pepin J, Levy P, Bonnet C, Perret JE, Pellat J, Feuerstein C (1995) Deficits of cognitive executive functions in patients with sleep apnea syndrome. Sleep 18:43–52
Kim HC, Young T, Matthews CG, Weber SM, Woodard AR, Palta M (1997) Sleep-disordered breathing and neuropsychological deficits. Am J Respir Crit Care Med 156:1813–1819
Aloia MS, Ilniczky N, Dio LD, Perlis ML, Greenblatt DW, Giles DE (2003) Neuropsychological changes and treatment compliance in older adults with sleep apnea. J Psychosom Res 54:71–76
Acknowledgements
Supported by the Telemedicine Directorate, Walter Reed Army Medical Center, Washington, DC.
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclosure Statement: Supported by the Telemedicine Directorate, Walter Reed Army Medical Center, Washington, DC.
Rights and permissions
About this article
Cite this article
Taylor, Y., Eliasson, A., Andrada, T. et al. The role of telemedicine in CPAP compliance for patients with obstructive sleep apnea syndrome. Sleep Breath 10, 132–138 (2006). https://doi.org/10.1007/s11325-006-0059-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-006-0059-9