Abstract
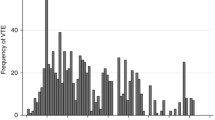
Cancer patients, especially those with lung cancer and undergoing chemotherapy, have an elevated risk for venous thromboembolism (VTE). This study assessed incidence, timing, and risk factors for VTE (specifically receipt of chemotherapy), along with the association between VTE and survival among lung cancer patients receiving chemotherapy. Using Florida Medicaid administrative claims data (2000–2008), patients with any diagnosis of primary lung cancer were selected. Patients with recent prior VTE and those enrolled in Medicare or an HMO were excluded. Crude rates of VTE per 100 person years were estimated, and Cox proportional hazards models were developed to assess risk factors for VTE in the lung cancer population, and the association between VTE and survival among patients undergoing chemotherapy. Of 15,749 lung cancer patients, 7,052 (2,242 receiving chemotherapy and 4,810 not receiving chemotherapy) met cohort selection criteria. The incidence of VTE was 10.8 per 100 person-years (PYs) in the chemotherapy cohort and 6.8 per 100 PYs in the non-chemotherapy cohort. Among patients on chemotherapy developing VTE, median time to occurrence was 109 days, with 61 and 82 % of patients experiencing an event within six and 12 months, respectively. In multivariate analyses, the adjusted risk of VTE was 30 % higher among patients undergoing chemotherapy. Comorbidity and the presence of a central venous catheter also were significantly associated with a greater risk of developing VTE. Moreover, patients in the chemotherapy cohort who developed VTE had a significantly faster time-to-death (adjusted hazard ratio [HR] = 1.97; 95 % CI 1.69–2.29).VTE was common among lung cancer patients, especially among patients receiving chemotherapy, with the majority of VTE events occurring within 6 months of initiation of chemotherapy. The presence of a VTE event was significantly associated with an increased risk of mortality.


Similar content being viewed by others
References
Chew HK, Davies AM, Wun T, Harvey D, Zhou H, White RH (2008) The incidence of venous thromboembolism among patients with primary lung cancer. J Thromb Haemost 6(4):601–608
Khorana AA, Francis CW, Culakova E, Kuderer NM, Lyman GH (2007) Frequency, risk factors, and trends for venous thromboembolism among hospitalized cancer patients. Cancer 110(10):2339–2346
Blom JW, Osanto S, Rosendaal FR (2004) The risk of a venous thrombotic event in lung cancer patients: higher risk for adenocarcinoma than squamous cell carcinoma. J Thromb Haemost 2(10):1760–1765
Bick RL (2003) Cancer-associated thrombosis. N Engl J Med 349(2):109–111
Khorana AA, Francis CW, Culakova E, Lyman GH (2005) Risk factors for chemotherapy-associated venous thromboembolism in a prospective observational study. Cancer 104(12):2822–2829
Khorana AA, Francis CW, Culakova E, Kuderer NM, Lyman GH (2007) Thromboembolism is a leading cause of death in cancer patients receiving outpatient chemotherapy. J Thromb Haemost 5(3):632–634
Paneesha S, Lokare A, Lester Z, Nokes T, Arya R, Farren T et al (2009) Impact of venous thromboembolism on survival in patients with malignancy. Br J Haematol 145(2):258–260
Sorensen HT, Mellemkjaer L, Olsen JH, Baron JA (2000) Prognosis of cancers associated with venous thromboembolism. N Engl J Med 343(25):1846–1850
Fotopoulou C, duBois A, Karavas AN, Trappe R, Aminossadati B, Schmalfeldt B et al. (2008) Incidence of venous thromboembolism in patients with ovarian cancer undergoing platinum/paclitaxel-containing first-line chemotherapy: an exploratory analysis by the Arbeitsgemeinschaft Gynaekologische Onkologie ovarian cancer study group. J Clin Oncol 26(16):2683–2689
Geerts WH, Bergqvist D, Pineo GF, Heit JA, Samama CM, Lassen MR et al (2008) Prevention of venous thromboembolism: American college of chest physicians evidence-based clinical practice guidelines (8th edn). Chest 133(6 Suppl):381S–453S
Lyman GH, Khorana AA, Falanga A, Clarke-Pearson D, Flowers C, Jahanzeb M et al (2007) American society of clinical oncology guideline: recommendations for venous thromboembolism prophylaxis and treatment in patients with cancer. J Clin Oncol 25(34):5490–5505
Blom JW, Doggen CJ, Osanto S, Rosendaal FR (2005) Malignancies, prothrombotic mutations, and the risk of venous thrombosis. J Am Med Assoc 293(6):715–722
Elting LS, Escalante CP, Cooksley C, Avritscher EB, Kurtin D, Hamblin L et al (2004) Outcomes and cost of deep venous thrombosis among patients with cancer. Arch Intern Med 164(15):1653–1661
Levitan N, Dowlati A, Remick SC, Tahsildar HI, Sivinski LD, Beyth R et al (1999) Rates of initial and recurrent thromboembolic disease among patients with malignancy versus those without malignancy. Risk analysis using Medicare claims data. Medicine (Baltimore) 78(5):285–291
Spyropoulos AC, Hussein M, Lin J, Battleman D (2009) Rates of venous thromboembolism occurrence in medical patients among the insured population. Thromb Haemost 102(5):951–957
White RH, Chew HK, Zhou H, Parikh-Patel A, Harris D, Harvey D et al (2005) Incidence of venous thromboembolism in the year before the diagnosis of cancer in 528,693 adults. Arch Intern Med 165(15):1782–1787
Florida Agency for Health Care Administration (2010) Medicaid, AHCA 2010. http://www.fdhc.state.fl.us/medicaid/. Accessed 29 November 2010
Hankin CS, Cox L, Lang D, Levin A, Gross G, Eavy G et al (2008) Allergy immunotherapy among medicaid-enrolled children with allergic rhinitis: patterns of care, resource use, and costs. J Allergy Clin Immunol 121(1):227–232
Hankin CS, Koran LM, Bronstone A, Black DW, Sheehan DV, Hollander E et al (2009) Adequacy of pharmacotherapy among medicaid-enrolled patients newly diagnosed with obsessive–compulsive disorder. CNS Spectr 14(12):695–703
Hankin CS, Cox L, Lang D, Bronstone A, Fass P, Leatherman B et al (2010) Allergen immunotherapy and health care cost benefits for children with allergic rhinitis: a large-scale, retrospective, matched cohort study. Ann Allergy Asthma Immunol 104(1):79–85
Marton JP, Boulanger L, Friedman M, Dixon D, Wilson J, Menzin J (2006) Assessing the costs of chronic obstructive pulmonary disease: the state medicaid perspective. Respir Med 100(6):996–1005
Lang K, Sussman M, Friedman M, Su J, Kan HJ, Mauro D et al (2009) Incidence and costs of treatment-related complications among patients with advanced squamous cell carcinoma of the head and neck. Arch Otolaryngol Head Neck Surg 135(6):582–588
Zhang B, Hepner DL, Tran MH, Friedman M, Korn JR, Menzin J (2009) Neuromuscular blockade, reversal agent use, and operating room time: retrospective analysis of US inpatient surgeries. Curr Med Res Opin 25(4):943–950
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40(5):373–383
Deyo RA, Cherkin DC, Ciol MA (1992) Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol 45(6):613–619
Duh MS, Reynolds WJ, Lefebvre P, Neary M, Skarin AT (2008) Costs associated with intravenous chemotherapy administration in patients with small cell lung cancer: a retrospective claims database analysis. Curr Med Res Opin 24(4):967–974
Suenaga M, Mizunuma N, Kobayashi K, Shinozaki E, Matsusaka S, Chin K et al (2010) Management of venous thromboembolism in colorectal cancer patients treated with bevacizumab. Med Oncol 27(3):807–814
Rasco DW, Yan J, Xie Y, Dowell JE, Gerber DE (2010) Looking beyond surveillance, epidemiology, and end results: patterns of chemotherapy administration for advanced non-small cell lung cancer in a contemporary, diverse population. J Thorac Oncol 5(10):1529–1535
Connolly GC, Dalal MR, Lin J, Khorana AA, University of Rochester RN, Sanofi-Aventis BN et al. (2011) Incidence and predictors of venous thromboembolism (VTE) among ambulatory patients with lung cancer. American Society of Clinical Oncology (ASCO). http://www.asco.org/ascov2/Meetings/Abstracts?&vmview=abst_detail_view&confID=102&abstractID=79817. Accessed 26 May 2011
de Meis E, Pinheiro VR, Zamboni MM, Guedes MT, Castilho IA, Martinez MM et al. (2009) Clotting, immune system, and venous thrombosis in lung adenocarcinoma patients: a prospective study. Cancer Invest 27(10):989–997
Numico G, Garrone O, Dongiovanni V, Silvestris N, Colantonio I, Di CG et al (2005) Prospective evaluation of major vascular events in patients with nonsmall cell lung carcinoma treated with cisplatin and gemcitabine. Cancer 103(5):994–999
Tagalakis V, Levi D, Agulnik JS, Cohen V, Kasymjanova G, Small D (2007) High risk of deep vein thrombosis in patients with non-small cell lung cancer: a cohort study of 493 patients. J Thorac Oncol 2(8):729–734
Schneeweiss S, Avorn J (2005) A review of uses of health care utilization databases for epidemiologic research on therapeutics. J Clin Epidemiol 53(327):337
Falanga A, Zacharski L (2005) Deep vein thrombosis in cancer: the scale of the problem and approaches to management. Ann Oncol 16(5):696–701
Thompson C, Rodgers R (1952) Analysis of the autopsy records of 157 cases of carcinoma of the pancreas with particular reference to the incidence of thromboembolism. Am J Med Sci 223:469–476
Acknowledgments
This study was sponsored by Daiichi Sankyo, Inc. Other than having an employee as a co-author, the funding source had no role in the interpretation or presentation of the data. The authors gratefully acknowledge Rick deFriesse at Boston Health Economics, Inc. for his assistance with data analysis.
Conflict of interest
Dr. Mallick is an employee of the study sponsor, Daiichi Sankyo, Inc. The rest of the authors have no financial disclosures.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Huang, H., Korn, J.R., Mallick, R. et al. Incidence of venous thromboembolism among chemotherapy-treated patients with lung cancer and its association with mortality: a retrospective database study. J Thromb Thrombolysis 34, 446–456 (2012). https://doi.org/10.1007/s11239-012-0741-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-012-0741-7