Abstract
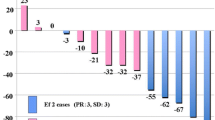
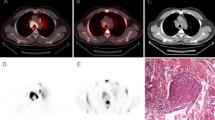
Thymomas are lacking in malignant cytological features. Their staging is defined by the invasiveness of the tumour. This study aimed to analyse the uptake patterns of fluorine-18 fluorodeoxyglucose (FDG) in thymomas of different stages. FDG positron emission tomography (PET) scan was performed in 12 patients suspected of having thymoma and in nine controls. Qualitative visual interpretation was used to detect the foci with FDG uptake higher than that of normal mediastinum. Tumour/lung ratio (TLR) was calculated from the counts of ROIs over the mass and over comparable normal lung tissue in thymoma patients. Mediastinum/lung ratio (MLR) was calculated from the counts of ROIs over the anterior mediastinum and lung in controls. The PET scan patterns of distribution of foci with FDG uptake and TLRs were correlated with the computed tomography (CT) or magnetic resonance imaging (MRI) findings, and staging of the thymomas. Thymectomy was performed in ten patients and thoracoscopy was done in two patients. The results revealed ten thymomas (two stage I tumours, two stage II, four stage III and two stage IV, according to the Masaoka classification), and two cases of thymic hyperplasia associated with myasthenia gravis. Myasthenia gravis was also noted in four thymoma patients. FDG studies showed (a) diffuse uptake in the widened anterior mediastinum in patients with thymic hyperplasia, (b) confined focal FDG uptake in the non-invasive or less invasive, stage I and II thymomas, and (c) multiple discrete foci of FDG uptake in the mediastinum and thoracic structures in stage III and IV advanced invasive thymomas. The thymomas had the highest TLRs, followed by the TLRs of thymic hyperplasia and the MLRs of control subjects (P <0.005). No significant difference was found between thymomas in different stages or between thymomas with and thymomas without myasthenia gravis. In comparison with CT and/or MRI, FDG-PET detected more lesions in patients with invasive thymomas and downgraded the staging of thymoma in four patients. Our preliminary results suggest that FDG-PET is useful in the assessment of the invasiveness of thymomas, and may have the potential to differentiate thymomas from thymic hyperplasia.
Similar content being viewed by others
References
Rosai J, Levine GD.Tumors of the thymus. Atlas of tumor pathology, 2nd series. Washington DC: Armed Forces Institute of Pathology, 1976: 34–153.
Batata MA, Martini N, Huvos AG, Agnilar RZ, Beattie EF Jr. Thymomas: clinicopathologic features, therapy and prognosis.Cancer 1974; 34: 389–396.
Watanabe H, Nakata H, Yoshimatsu H. CT diagnosis of malignant thymoma [in Japanese].Sangyo Ika Daigaku Zasshi 1986; 8: 437–442.
Sakai F, Sone S, Kiyono K, et al. MR imaging of thymoma: radiologic-pathologic correlation.AJR 1992; 158: 751–756.
Molina PL, Siegel MJ, Glazer HS. Thymic masses on MR imaging.AJR 1990; 155: 495–500.
Lee JD, Choe KO, Kim SJ, Kim GE, Im JG, Lee JT. CT findings in primary thymic carcinoma.J Comput Assist Tomogr 1991; 15: 429–433.
Gorich J, Muller M, Beyer-Enke SA, Zuna I, Probst G, van Kaick G. Computed tomographic findings in 36 patients with space-occupying lesions of the thymus [in German].Nuklearmedizin 1988; 149: 466–469.
Masaoka A, Yasumasa M, Nakahara K, Tanioka T. Follow-up study of thymomas with special reference to their clinical stages.Cancer 1981; 48: 2485–2492.
Wang LS, Huang MH, Lin TS, Huang BS, Chien KY. Malignant thymoma.Cancer 1992; 70: 443–450.
Zerhouni EA, Scott W Jr, Baker RR, Wharam MO, Siegelman SS. Invasive thymomas: diagnosis and evaluation by computed tomography.J Comput Assist Tomogr 1982; 6: 92–100.
Shields TW, Fox RT, Lees WM. Thymic tumors: classification and treatment.Arch Surg 1996; 92: 617–622.
Siegel MJ. Diseases of the thymus in children and adolescents.Postgrad Radiol 1993; 13: 106–132.
Batra P, Hermann C Jr, Mulder D. Mediastinal imaging in myasthenia gravis: correlation of chest radiography, CT, MR, and surgical findings.AJR 1987; 148: 515–519.
Baron RL, Lee JKT, Sagel SS, Levitt RG. Computed tomography of the abnormal thymus.Radiology 1982; 142: 127–134.
Siegel MJ. Chest applications of magnetic resonance imaging in children.Top Magn Reson Imaging 1990; 3: 1–23.
Kim EE, Haynie TP, Kim BT. Biochemical imaging in the management of cancer.Am J Physiol Imaging 1992; 314: 199–202.
Strauss LG, Conti PS. The applications of PET in clinical oncology.J Nucl Med 1991; 32: 623–648.
Hawkins RA, Hoh CK, Dahlborn M, et al. PET cancer evaluations with FDG.J Nucl Med 1991; 32: 1555–1558.
Hawkins RA, Choi Y, Huang S-C, Messa C, Hoh CK, Phelps ME. Quantitating tumor glucose metabolism with FDG and PET.J Nucl Med 1992; 33: 339–344.
Kubota K, Matsuzawa T, Fujiwara T, et al. Differential diagnosis of lung tumor with positron emission tomography: a prospective study.J Nucl Med 1990; 31: 1927–1933.
Jabour BA, Choi Y, Hoh CK, et al. Extracranial head and neck: PET imaging with 2-[F-18]fluoro-2-deoxy-D-glucose and MR imaging correlation.Radiology 1993; 186: 27–35.
Kubota RK, Yamada S, Kubota K, et al. Intratumoral distribution of fluorine-18-fluorodeoxyglucose in vivo: high accumulation in macrophages and granulation tissues studied by microautoratiography.J Nucl Med 1992; 33: 1972–1980.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Liu, RS., Yeh, SH., Huang, MH. et al. Use of fluorine-18 fluorodeoxyglucose positron emission tomography in the detection of thymoma: A preliminary report. Eur J Nucl Med 22, 1402–1407 (1995). https://doi.org/10.1007/BF01791148
Received:
Revised:
Issue Date:
DOI: https://doi.org/10.1007/BF01791148