Abstract
Background
Continuous positive airway pressure treatment has been shown to lower blood pressure (BP) in patients with obstructive sleep apnea (OSA). The aims of the present pilot study were to evaluate the potential effects of oral appliance (OA) therapy on BP, to assess various outcome BP measures, and to inform sample size calculation.
Methods
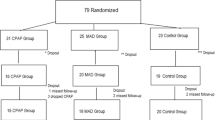
Seventy-two patients with OSA and hypertension were randomly assigned to intervention with either an OA with mandibular advancement (active group) or an OA without advancement (control group). Before and after 3 months of treatment, the patients underwent nocturnal somnographic registration and 24-h ambulatory BP monitoring.
Results
Among the various BP measures, the largest trend toward effect of OA treatment was seen in 24-h mean systolic BP with a 1.8 mmHg stronger BP reduction in the active group compared with controls. A stronger trend toward effect was seen in a subgroup with baseline ambulatory daytime mean systolic BP >135/85 mmHg where the mean systolic BP fell, on average, 2.6 mmHg. Additional exclusion of patients with baseline apnea hypopnea index (AHI) ≤15 gave a significant reduction in mean systolic BP of 4.4 mmHg (P = 0.044) in the active group compared with controls.
Conclusions
In patients with OSA and hypertension, OA treatment had a modest trend toward effect on reducing BP. A stronger trend toward treatment effect was seen after excluding patients with normal baseline ambulatory BP. Additional exclusion of patients with baseline AHI ≤15 showed a significant treatment effect. Data to inform sample size for an adequately powered randomized study are provided.



Similar content being viewed by others
References
Somers VK, White DP, Amin R, Abraham WT, Costa F, Culebras A, Daniels S, Floras JS, Hunt CE, Olson LJ, Pickering TG, Russell R, Woo M, Young T (2008) Sleep apnea and cardiovascular disease. Circulation 118(10):1080–1111
Shah NA, Yaggi HK, Concato J, Mohsenin V (2010) Obstructive sleep apnea as a risk factor for coronary events or cardiovascular death. Sleep Breathing 14(2):131–136
Bixler EO, Vgontas AN, Lin H-M, Have TT, Rein J, Vela-Bueno A, Kales A (2001) Prevalence of sleep-disordered breathing in women. Am J Respir Crit Care Med 163(3):608–613
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328(17):1230–1235
Davies RJ, Belt PJ, Roberts SJ, Ali NJ, Stradling JR (1993) Arterial blood pressure responses to graded transient arousal from sleep in normal humans. J Appl Physiol 74(3):1123–1130
Peppard PE, Young T, Palta M, Skatrud J (2000) Prospective study of the association between sleep-disordered breathing and hypertension. N Engl J Med 342(19):1378–1384
Lavie P, Herer P, Hoffstein V (2000) Obstructive sleep apnoea syndrome as a risk factor for hypertension: population study. BMJ 320(7233):479–482
Nieto FJ, Young TB, Lind BK, Shahar E, Samet JM, Redline S, D'Agostino RB, Newman AB, Lebowitz MD, Pickering TG (2000) Association of sleep-disordered breathing, sleep apnea, and hypertension in a large community-based study. JAMA 283(14):1829–1836
Yaggi HK, Concato J, Kernan WN, Lichtman JH, Brass LM, Mohsenin V (2005) Obstructive sleep apnea as a risk factor for stroke and death. New Engl J Med 353(19):2034–2041
Marin JM, Carrizo SJ, Vicente E, Agusti AGN (2005) Long-term cardiovascular outcomes in men with obstructive sleep apnoea–hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet 365(9464):1046–1053
Shahar E, Whitney C, Redline S, Lee E, Newman A, JavierNieto F, O’Connor G, Boland L, Schwartz J, Samet J (2001) Sleep-disordered breathing and cardiovascular disease. Am J Resp Crit Care Med 163(1):19–25
Faccenda J, Mackay T, Boon N, Douglas N (2001) Randomized placebo-controlled trial of continuous positive airway pressure on blood pressure in the sleep apnea–hypopnea syndrome. Am J Resp Crit Care Med 163(2):344–348
Pepperell JCT, Ramdassingh-Dow S, Crosthwaite N, Mullins R, Jenkinson C, Stradling JR, Davies RJO (2002) Ambulatory blood pressure after therapeutic and subtherapeutic nasal continuous positive airway pressure for obstructive sleep apnoea: a randomised parallel trial. Lancet 359(9302):204–210
Bazzano LA, Khan Z, Reynolds K, He J (2007) Effect of nocturnal nasal continuous positive airway pressure on blood pressure in obstructive sleep apnea. Hypertension 50(2):417–423
Mehta A, Qian J, Petocz P, Darendeliler MA, Cistulli P (2001) A randomized, controlled study of a mandibular advancement splint for obstructive sleep apnea. Am J Resp Crit Care Med 163(6):1457–1461
Walker-Engström M-L, Tegelberg Å, Wilhelmsson B, Ringqvist I (2002) 4-year follow-up of treatment with dental appliance or uvulopalatopharyngoplasty in patients with obstructive sleep apnea. Chest 121(3):739–746
Aarab G, Lobbezoo F, Hamburger HL, Naeije M (2011) Oral appliance therapy versus nasal continuous positive airway pressure in obstructive sleep apnea: a randomized, placebo-controlled trial. Respiration 81(5):411–419
Otsuka R, Ribeiro de Almeida F, Lowe A, Linden W, Ryan F (2006) The effect of oral appliance therapy on blood pressure in patients with obstructive sleep apnea. Sleep Breathing 10(1):29–36
Yoshida K (2006) Effect on blood pressure of oral appliance therapy for sleep apnea syndrome. Int J Prosthodont 19(1):61–66
Andrén A, Sjöquist M, Tegelberg Å (2009) Effects on blood pressure after treatment of obstructive sleep apnoea with a mandibular advancement appliance—a three-year follow-up. J Oral Rehabil 36(10):719–725
Gotsopoulos H, Kelly JJ, Cistulli PA (2004) Oral appliance therapy reduces blood pressure in obstructive sleep apnea: a randomized, controlled trial. Sleep 27(5):934–941
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14(6):540–545
Tegelberg A, Wilhelmsson B, Walker-Engstrom ML, Ringqvist M, Andersson L, Krekmanov L, Ringqvist I (1999) Effects and adverse events of a dental appliance for treatment of obstructive sleep apnoea. Swed Dent J 23(4):117–126
Ng SSS, Chan T-O, To K-W, Ngai J, Tung A, Ko FWS, Hui DSC (2010) Validation of Embletta portable diagnostic system for identifying patients with suspected obstructive sleep apnoea syndrome (OSAS). Respirology 15(2):336–342
Jones SC, Bilous M, Winship S, Finn P, Goodwin J (2004) Validation of the OSCAR 2 oscillometric 24-hour ambulatory blood pressure monitor according to the International Protocol for the validation of blood pressure measuring devices. Blood Press Monit 9(4):219–223
O'Brien E, Asmar R, Beilin L, Imai Y, Mallion JM, Mancia G, Mengden T, Myers M, Padfield P, Palatini P, Parati G, Pickering T, Redon J, Staessen J, Stergiou G, Verdecchia P, European Society of Hypertension Working Group on Blood Pressure (2003) European Society of Hypertension recommendations for conventional, ambulatory and home blood pressure measurement. J Hypertens 21(5):821–848
Grote L, Ploch T, Heitmann J, Knaack L, Penzel T, Peter JH (1999) Sleep-related breathing disorder is an independent risk factor for systemic hypertension. Am J Resp Crit Care Med 160(6):1875–1882
MacMahon S, Peto R, Cutler J, Collins R, Sorlie P, Neaton J, Abbott R, Godwin J, Dyer A, Stamler J (1990) Blood pressure, stroke, and coronary heart disease. Part 1, prolonged differences in blood pressure: prospective observational studies corrected for the regression dilution bias. Lancet 335(8692):765–774
Lim J, Lasserson TJ, Fleetham J, Wright J (2004) Oral appliances for obstructive sleep apnoea. Cochrane Database Syst Rev (4):CD004435
Hoekema A, Stegenga B, De Bont LG (2004) Efficacy and co-morbidity of oral appliances in the treatment of obstructive sleep apnea–hypopnea: a systematic review. Crit Rev Oral Biol Med 15(3):137–155
Franklin K, Rehnqvist N, Axelsson S (2007) Obstructive sleep apnoea syndrome—report of a joint Nordic project. A systematic review. Swedish Council on Health Technology Assessment, Stockholm
Collins R, Peto R, MacMahon S, Hebert P, Fiebach NH, Eberlein KA, Godwin J, Qizilbash N, Taylor JO, Hennekens CH (1990) Blood pressure, stroke, and coronary heart disease. Part 2, short-term reductions in blood pressure: overview of randomised drug trials in their epidemiological context. Lancet 335(8693):827–838
Krause T, Lovibond K, Caulfield M, McCormack T, Williams B (2011) Management of hypertension: summary of NICE guidance. BMJ 343:d4891
Verdecchia P, Angeli F, Mazzotta G, Gentile G, Reboldi G (2009) Home blood pressure measurements will not replace 24-hour ambulatory blood pressure monitoring. Hypertension 54(2):188–195
Wilhelmsson B, Tegelberg A, Walker-Engstrom ML, Ringqvist M, Andersson L, Krekmanov L, Ringqvist I (1999) A prospective randomized study of a dental appliance compared with uvulopalatopharyngoplasty in the treatment of obstructive sleep apnoea. Acta Otolaryngol 119(4):503–509
Walker-Engstrom ML, Ringqvist I, Vestling O, Wilhelmsson B, Tegelberg A (2003) A prospective randomized study comparing two different degrees of mandibular advancement with a dental appliance in treatment of severe obstructive sleep apnea. Sleep Breathing 7(3):119–130
Kato J, Isono S, Tanaka A, Watanabe T, Araki D, Tanzawa H, Nishino T (2000) Dose-dependent effects of mandibular advancement on pharyngeal mechanics and nocturnal oxygenation in patients with sleep-disordered breathing. Chest 117(4):1065–1072
Acknowledgments
The project was financially supported by grants from the County of Västmanland, Sweden, the Swedish Heart and Lung Foundation, and the Swedish Dental Association.
The authors wish to thank Yvonne Pettersson, dental assistant, for her active role in the administration and rolling of the patients.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Andrén, A., Hedberg, P., Walker-Engström, ML. et al. Effects of treatment with oral appliance on 24-h blood pressure in patients with obstructive sleep apnea and hypertension: a randomized clinical trial. Sleep Breath 17, 705–712 (2013). https://doi.org/10.1007/s11325-012-0746-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-012-0746-7