Article Text
Abstract
Background: The optimal way of assessing the impact of pulmonary rehabilitation on functional status in chronic obstructive pulmonary disease (COPD) is currently unknown. The minimal clinically important difference for the constant work rate cycling exercise test also needs to be investigated to facilitate its interpretation. A study was undertaken to evaluate the changes in the 6-min walking test and in the constant work rate cycle endurance test immediately following and 1 year after pulmonary rehabilitation, together with the importance of these changes in terms of health status in patients with COPD.
Methods: Patients with COPD of mean (SD) age 65 (8) years and mean (SD) forced expiratory volume in 1 s (FEV1) 45 (15)% predicted were recruited from a multicentre prospective cohort study and evaluated at baseline, immediately after a pulmonary rehabilitation programme (n = 157) and at 1 year (n = 106). The 6-min walking test and the cycle endurance test were performed at each evaluation. Health status was evaluated with the St George Respiratory Questionnaire.
Results: Following pulmonary rehabilitation, cycle endurance time increased (198 (352) s, p<0.001) and stayed over baseline values at 1 year (p<0.001). The 6-min walking distance also showed improvements following rehabilitation (25 (52) m, p<0.001) but returned to baseline values at the 1-year follow-up. Changes in cycle endurance time were more closely associated with changes in health status than with the 6-min walking test. An improvement of 100–200 s in the cycle endurance time was associated with clinically meaningful changes in the St George Respiratory Questionnaire scores.
Conclusions: The cycle endurance test was more responsive than the 6-min walking test in detecting improvement in exercise tolerance following pulmonary rehabilitation, and was also better correlated with improvements in health status. An improvement in the cycle endurance time of 100–200 s appeared to be clinically meaningful.
Statistics from Altmetric.com
Exercise intolerance is a foremost complaint in patients with chronic obstructive pulmonary disease (COPD) and is associated with decreased quality of life and survival.1 Exercise capacity in COPD may be evaluated using walking or cycling exercise protocols. While maximal progressive cycle tests are more widely used,2–4 cycling or walking endurance protocols are gaining popularity and have shown responsiveness to bronchodilation5 6 and pulmonary rehabilitation.7 8 The 6-min walking test (6MWT) is also a commonly employed test used to assess functional capacity in COPD,9 although its responsiveness to interventions such as bronchodilation10 and pulmonary rehabilitation11 may not be optimal.
The current literature suggests that the cycle endurance test (CET) is more responsive to detect improvement in functional capacity immediately after pulmonary rehabilitation than the 6MWT.2 12 13 Despite this notion, the 6MWT is still largely used to evaluate the effects of pulmonary rehabilitation because of its simplicity and ease of administration.9 Furthermore, the 6MWT has demonstrated clinical significance compared with the CET, which has yet to show similar importance.
One interesting feature of the 6MWT which also contributes to its popularity is the knowledge of a minimal clinically important difference, key information when interpreting the results of a given test. Redelmeier and colleagues14 have reported that a change in the 6 min distance walked of 54 m (95% confidence interval (CI) 37 to 71) is likely to be perceived by patients. Although a similar evaluation has not been reported for the constant work rate cycling exercise test, Casaburi15 recently proposed that a minimal improvement of 105 s in the endurance time of the CET should be considered as clinically meaningful. This estimate was derived from a study by O’Donnell et al16 on the effects of bronchodilation on constant work rate endurance time, and from the fact that an improvement in endurance time of more than half the SD of the change in endurance time has a high likelihood of being clinically important.17 Whether a similar estimate would be obtained in a study relating the changes in cycling endurance time to those of health status assessment following pulmonary rehabilitation is unclear. This is an important research question; if the endurance time to constant work rate cycling exercise is to become widely used, a clinically significant threshold needs to be established for this parameter.
The present study was undertaken to test the hypothesis that the CET would be more responsive to rehabilitation than the 6MWT immediately following the intervention and after 1 year of follow-up. We also hypothesised that the changes in the endurance time in the CET seen after rehabilitation would be clinically meaningful, as indicated by correlation analyses with the changes in health status. Lastly, we felt that it would be possible to identify a minimal clinically important difference for the changes in the endurance time to constant work rate cycling exercise. To address these issues, we used a multicentre prospective cohort of patients with COPD entering pulmonary rehabilitation in the province of Quebec, Canada.
METHODS
Subjects and study design
One hundred and sixty-eight patients with moderate to severe COPD were recruited in two centres (Hôpital Laval in Quebec City and Montreal Chest Institute in Montreal, Canada). Patients were part of a prospective cohort entering pulmonary rehabilitation initiated in the province of Quebec with the intention of testing a number of hypotheses regarding the responsiveness of the 6MWT and the CET to rehabilitation. Inclusion criteria were: clinical diagnosis of COPD for at least 4 weeks, incompletely reversible airflow obstruction (post-bronchodilator forced expiratory volume in 1 s/forced vital capacity (FEV1/FVC) <70%), no asthma, heart failure, dementia or unstable psychological conditions. Patients were required to have completed the baseline evaluation (before rehabilitation) and at least one evaluation after rehabilitation (immediately after and/or 1 year after). Patients’ assessment included a complete medical history, pulmonary function tests at rest, CET, 6MWT and health status as measured by the St George Respiratory Questionnaire (SGRQ). Patients were included if they had not participated in a pulmonary rehabilitation programme in the past 12 months and were in a stable state (ie, no exacerbation of their disease in the preceding month) at study entry.
The rehabilitation programme consisted of 6–12 weeks of 3-weekly 90 min exercise sessions that integrated endurance training (cycling and walking), muscle strengthening exercises and patient education, which has been described in detail elsewhere.18 There was no formal maintenance programme after the 6–12 weeks of rehabilitation. The study procedures were standardised by one of the investigator (SB) who monitored the study sites. All patients gave informed consent to participate in the study. The ethics committees from the two study sites approved the research project.
Pulmonary function testing
Spirometry and lung volumes were measured according to recommended procedures.19 The results were compared with predicted normal values from the European Community for Coal and Steel/European Respiratory Society.20
Incremental cycle ergometry
Peak cycling capacity was determined with progressive cycle ergometry with workload increments of 10 watts/minute until exhaustion.21 Peak work capacity was related to the normal values of Jones et al.21
Cycle endurance test (CET)
The CET was performed on an electromagnetically braked cycle ergometer and the workload was set at 80% of peak work capacity achieved during incremental cycle ergometry. Patients were asked to cycle for as long as possible and no encouragement was provided during the tests to avoid any potential confounding effect on exercise performance.22
Six-minute walking test (6MWT)
The 6MWT was administered in an enclosed corridor in accordance with the procedures recommended by the American Thoracic Society (ATS),9 except for the course which was 20 m long and the addition of a practice walk. An elliptical walking course was used at both research centres. Before each test, patients were instructed to cover as much ground as possible in the allotted time period. Patients were also notified that no encouragement would be provided to them during the test, but that they would be kept aware of time, in accordance with the ATS guidelines.9
Health status
Health status was evaluated using a formally validated French version of the SGRQ.23 The SGRQ is a disease-specific measure that has been extensively validated in patients with all grades of respiratory disease including advanced COPD.24 The questionnaire consists of 76 items divided into three domains (symptoms, activity and impact). Scores range from 0 (perfect health) to 100 (worst possible) for each component; a total score which summarises the responses to all items is obtained. A change in score of 4 units may be considered clinically significant.
Statistical analysis
Results are reported as mean (SD). A p value <0.05 was considered statistically significant. Paired t tests were used to evaluate the comparative sensitivity of the CET and the 6MWT to detect improvements induced by pulmonary rehabilitation. Pearson correlations were calculated between baseline SGRQ scores and both the endurance time to CET and distance walked during the 6MWT, and also between changes in SGRQ scores and changes in endurance time to CET and distance walked during the 6MWT.
Two approaches were used to define a minimal clinically important difference (MCID) or range for the CET. The first method—the anchor-based approach—related changes in the endurance time to CET to those of the SGRQ total scores. Changes immediately after rehabilitation and at 1 year were pooled for this analysis (n = 263 observations). The SGRQ is a validated health status instrument24 for which a negative change of ⩾4 units is clinically important. Cycle endurance time improvements (dependent variable) were plotted with improvements in SGRQ (independent variable) in a linear regression and the 95% confidence interval (CI) of endurance time yielding an improvement of at least 4 units in SGRQ was calculated.25
The second method—the distribution-based approach—to assess the MCID is based on the observations that half the standard deviation of the change in a given variable has a high likelihood of being perceived by the subjects.26 The MCID range for the CET was categorised into a lower, intermediate and upper boundary.
The validity of the estimated MCID for the CET was separately tested in 52 patients with COPD who were not involved in the original analysis (they were subsequently recruited). These patients fulfilled the inclusion/exclusion criteria of the study and also participated in the prospective cohort. These patients completed baseline and immediately post-rehabilitation and/or 1 year follow-up visits after analyses for this study were completed. We calculated the mean difference in the change in endurance time to CET between patients showing a change in SGRQ of ⩽−4 units (improvement) and patients with a change in SGRQ of >−4 units (no improvement or deterioration).
The effect size for each of the different estimates of the MCID of the CET was obtained by dividing the average change in SGRQ total score (post − pre-rehabilitation value) by the standard deviation of the baseline value (pre-rehabilitation) for this variable.27 An effect size of 0.20 indicates a small change, while effect sizes of 0.50 and 0.80 denote moderate and large changes, respectively.28 Patients were separated according to their response to the 6MWT and CET into those showing no clinically meaningful improvement in both tests, those improving only on the 6MWT, those improving only on the CET, and those showing clinically meaningful improvement to both the 6MWT and the CET. A significant clinical improvement was defined as ⩾54 m for the 6MWT14 and 100 s for the CET. SGRQ improvements following rehabilitation for the four groups were compared using an ANOVA.
RESULTS
Patient characteristics
Of the 168 patients who fulfilled the inclusion criteria, 157 (93%) completed the baseline and post-rehabilitation evaluation and 106 (63%) completed the baseline and 1-year follow-up. Of the 157 patients who completed baseline and post-rehabilitation evaluations, 62 were not evaluated at 1 year: 2 had died, 12 dropped out, in 34 cases one of the three tests needed for the study was missing and 14 had not yet completed the 1-year evaluation. Eleven patients could not be evaluated immediately after rehabilitation (because of a COPD exacerbation or unable to schedule the visit) and were evaluated only at the 1-year follow-up. The characteristics of the study group are shown in table 1. Patients had on average moderate to severe airflow obstruction and markedly limited exercise capacity.
Changes in exercise capacity and health status following pulmonary rehabilitation
Improvements in CET, 6MWT and SGRQ immediately following the rehabilitation programme and at 1-year follow-up are shown in table 2 and fig 1. The mean improvement in the 6MWT was smaller than the reported MCID for this parameter (54 m, 95% CI 37 to 71). Immediately after rehabilitation, 43 (27%) subjects had a clinically significant improvement in their walking distance (>54 m).
There was a statistically and clinically (⩾4 units) significant improvement in all domains of the SGRQ immediately after completing the rehabilitation program and at one year except for the activity domain (table 2).
The correlations between baseline exercise values and SGRQ scores are shown in table 3, and the correlations between the changes in measures of exercise capacity and those in health status are shown in table 4.
Baseline SGRQ scores correlated with the CET and 6MWT (table 3). There was no correlation between the changes in SGRQ scores and the 6MWT, but the changes in endurance time to CET correlated moderately with changes in SGRQ scores (table 4).
Minimally clinically important difference (MCID)
A linear regression analysis was performed between changes in SGRQ total scores and endurance time to CET for the pooled changes immediately after rehabilitation and at 1 year follow-up (n = 263). The slope of this relationship was −9.21 s (95% CI −12.9 to −5.6) and the intercept was 116.4 s (95% CI 70.8 to 162.1) which indicates that, for an individual to show a clinically meaningful improvement in the SGRQ (at least 4 units), a variation of 153 s (95% CI 93 to 213) in endurance time to CET was necessary. A similar analysis could not be performed for the 6MWT since changes in 6MWT were not significantly correlated with changes in SGRQ scores. A 170 s change in endurance time to CET was estimated to represent the clinically significant threshold based on the half standard deviation approach. Among the 52 patients in whom this MCID estimate for CET was subsequently tested, 29 completed baseline and post-rehabilitation evaluations and 39 completed the baseline and 1 year follow-up evaluations (a total of 68 pairs of data). Mean (SD) age (67 (8) years) and FEV1 (1.01 (0.28) l; 45 (16)% predicted) were similar to those of the 168 patients involved in the initial analysis. The mean difference in CET between patients showing a change in the SGRQ of ⩽−4 (improvement) and those in whom the change in SGRQ was >−4 (no improvement or deterioration) was 178 s (p<0.05), consistent with our MCID estimate for this parameter.
Table 5 shows the mean changes in CET and SGRQ total scores obtained in patients reaching the lower (100 s), intermediate (150 s) and upper (200 s) boundaries of the clinically significant range for the CET. The corresponding effect size for the improvement in the SGRQ is also shown.
Clinical significance of change in measures of exercise capacity
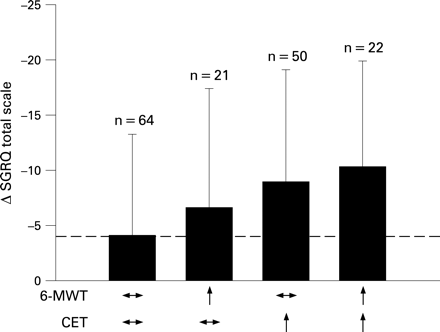
Using an improvement in the CET of 100 s and an improvement for the 6MWT of 54 m as the respective clinically significant thresholds for these two measures of exercise capacity,14 subjects were separated into responders and non-responders for each exercise test, thus resulting in four categories of patients (fig 2). Immediately following the rehabilitation programme, approximately one-third of the patients did not show any clinically meaningful improvement to either test after rehabilitation. Despite this, these individuals had, on average, an improvement in the SGRQ total score of 4.3 units. More than twice as many patients showed a clinically meaningful improvement in the CET without improving the 6MWT (n = 50) compared with patients with no meaningful improvement in the CET despite a clinically meaningful improvement in the 6MWT (n = 21). Patients exhibiting an increase only in the 6MWT had an improvement in the SGRQ total score of 6.6 units. Patients with improvement only in the CET or in the CET and the 6MWT had a large average gain in the SGRQ score (8.9 units). When using the lower boundary for the MCID of the 6MWT (37 m),14 44 patients improved only on the CET and 29 only on the 6MWT, corresponding to improvements on the SGRQ total score of −9.7 (10.3) units and −6.0 (10.4) units, respectively. The conclusions from fig 2 therefore remain whether the mean value or the lower boundary of the 95% CI of the MCID for the 6MWT was used in the analysis. The progressively greater improvement in the SGRQ total score when going from no improvement in measures of exercise capacity to clinically meaningful changes in both exercise tests was statistically significant (p<0.001). The proportion of patients showing an improvement in SGRQ total score of ⩾4 units in the subgroups showing no improvement in both exercise tests, improving only on the 6MWT, improving only on the CET and improving on both tests was 53%, 67%, 68% and 91%, respectively (p<0.05).
DISCUSSION
The objectives of this study were to compare the responsiveness of the 6MWT and of the CET to detect changes following pulmonary rehabilitation and to identify a clinically significant threshold for the CET in patients with COPD. Our results can be summarised as follow: (1) the CET is more sensitive to the acute and long-term effects of pulmonary rehabilitation than the 6MWT; (2) the improvements in CET correlated with gains in health status while the changes in 6MWT did not; (3) a change in the cycle endurance time of 100–200 s was associated with clinically significant improvements in health status as assessed by the SGRQ.
Few studies have compared the effects of pulmonary rehabilitation on the 6MWT and the CET, but available reports2 13 29 reported much larger improvements in cycle endurance time than in the 6MWT. Taken together, these studies and ours clearly indicate that the 6MWT is not the best tool to evaluate the efficacy of pulmonary rehabilitation. Having confirmed a greater responsiveness of the CET over the 6MWT, one may wonder about the clinical significance of improvement only in the CET when no changes are observed in the 6MWT. The present study supports the idea that the modifications in the CET are clinically relevant since they are associated with improvement in health status (table 5, fig 2) even in the absence of a significant change in the 6MWT. These findings have practical implications in evaluating the overall response to pulmonary rehabilitation.
An emerging discussion in pulmonary rehabilitation concerns the observation that some patients with COPD do not seem to respond to this intervention.30 The present results underscore the difficulty in addressing the important issue of response versus non-response to pulmonary rehabilitation. For instance, relying solely on the 6MWT to assess the response to pulmonary rehabilitation will lead to a gross underestimation of the response rate. We would therefore suggest that the response to rehabilitation should not be defined based on only one parameter, but rather on a combination of factors that should include a constant work rate exercise protocol.
The absence of a correlation between changes in 6MWT and changes in SGRQ total scores found in the present study are consistent with a previous report.31 In contrast, the baseline values of the 6MWT and of the SGRQ total scores were significantly correlated. These results are consistent with the current knowledge about the 6MWT. The distance walked during a 6-min period is statistically associated with health status32 and is a good predictor of mortality,33 indicating adequate discriminative properties of the test. On the other hand, the responsiveness of the 6MWT, a self-paced walking test, is smaller than that of externally paced walking or cycling protocols,10 34 indicating suboptimal evaluating properties. It is becoming clear in the field of COPD that the clinical use of the 6MWT should be to assess disease severity (discriminative properties) and prognosis (predictive properties) but not to evaluate response to treatment.
An exploration of the mechanisms explaining the differences in responsiveness to rehabilitation between the 6MWT and the CET was beyond the scope of the present study. The 6MWT is a self-paced test (ie, patients determine their own walking speed) with a fixed duration. Patients may learn to self-pace in pulmonary rehabilitation which could also influence responsiveness. In contrast, the CET is an externally paced test (ie, work load is dictated to patients) with an indefinite duration. Accordingly, improvements in performance are achieved differently for the two tests. Patients have to increase walking speed to cover more distance on the 6MWT while they have to increase endurance time to achieve the same outcome on the CET.
In a previous study evaluating the responsiveness of the 6MWT to acute bronchodilation,10 cardiorespiratory kinetics and walking speeds were remarkably similar during two 6MWTs performed on separate days, indicating that patients reproduce the same walking pattern during repeated 6-min walking. In the present study the improvement in the 6MWT was small but consistent, with the magnitude of improvement usually seen after rehabilitation35 suggesting that changing walking speed is a difficult goal to achieve in this setting. In contrast, patients were more likely to increase their cycling endurance time after rehabilitation. These findings indicate that it is easier to increase endurance time than to modify walking pattern, thereby suggesting that the different designs of the two tests had an impact on their respective response to bronchodilation.
The changes in cycle endurance time in the CET are currently difficult to interpret given the lack of data relating the changes in this parameter with patient-centered outcomes such as health status. There is no convention as to which method is preferable to compute a MCID value. However, some authors36 have suggested that the use of only one method is likely to result in imprecision and that combining statistical estimates with clinically-based anchors is recommended. Combining the anchor and distribution-based approaches as well as other data,15 we found that an improvement of 100–200 s in the cycle endurance time is clinically relevant. In 52 additional patients not involved in the original analysis, the mean difference in endurance time in the CET between patients who improved SGRQ and those who did not was 178 s, a value comprised within the confidence interval of our estimate. Based on the findings that an improvement of 100 s in cycle endurance time (the lower estimate of the clinically relevant zone) was associated with large gains in health status, we propose that an intervention associated with such an improvement in the CET should be viewed as clinically relevant.
Study limitations
We used the anchor-based approach in correlating the changes in the endurance time in the CET to those of the SGRQ total scores as an attempt to estimate the minimal important difference for the CET. The precision of this estimate is obviously dependent on the tightness of the correlation between the target instrument (CET) and the anchor (SGRQ).37 In the present study this correlation was modest (r = −0.31), but in the expected range for a correlation between physiological and health status measurements. Because of the imprecision inherent in this method of assessing the minimal clinically significant difference, we felt that it was more appropriate to report a range (100–200 s) of clinically meaningful improvements based on the 95% CI of the regression analysis between the changes in the CET and in the SGRQ than reporting only a discrete threshold. This information should help in interpreting the results of clinical trials reporting the effects of interventions aimed at improving functional status as assessed by the endurance time in the CET. Another potential limitation of the present study is that we cannot be absolutely certain whether our estimation of the MCID for the CET would also apply to pharmacological interventions since all measurements were obtained during rehabilitation. It is, however, reassuring that, using data collected during a pharmacological trial, it was estimated that the MCID for the CET was 105 s, an improvement which falls into the range proposed in the present study.
In summary, the present study provides clinically useful information about the assessment of the impact of pulmonary rehabilitation in patients with COPD. We first confirmed the greater responsiveness of the CET over the 6MWT. More importantly, in a significant proportion of patients with COPD, improvements in the CET were seen without changes in the 6MWT. This finding was clinically relevant, as suggested by the clear association with changes in health status. Lastly, a gain of 100 s (range 100–200 s) in the CET is proposed as a clinically meaningful difference for this exercise test.
Acknowledgments
The authors acknowledge the help of Marthe Bélanger, Brigitte Jean, Josée Picard, Hanèn N’Kaouar and Palmina Mancino in accomplishing this study. They also thank Yvan Fortier, Danielle Picard, Denise Légaré and Micheline Paquin for their work on the database and Serge Simard for his statistical assistance.
REFERENCES
Footnotes
-
None.
-
LL is supported by a PhD award from the Centre de Recherche de l’Hôpital Laval. JB is the recipient of a John R & Clara Fraser Memorial Award from the faculty of Medicine, McGill University. VP is supported by la Fondation de l’Hôpital du Sacré-Cœur de Montréal. FM is a research scholar of the Fonds de la Recherche en Santé du Québec. This work was supported by the Respiratory Health Network of the FRSQ and by an unrestricted grant from GlaxoSmithKline, Canada.