Article Text
Abstract
Yellow nail syndrome is a type of lymphatic dysplasia syndrome characterised by the triad of yellow nails, lymphoedema, and pleural effusions. The case history is presented of a 70 year old patient with yellow nail syndrome who complained of dyspnoea caused by massive chylothorax. The patient underwent insertion of a pleuroperitoneal shunt which resulted in abdominal distension and deterioration of leg oedema. The pleuroperitoneal shunt was replaced by a pleurovenous shunt on the right side which led to an improvement in the bilateral pleural effusions, abdominal distension, and leg oedema. A pleurovenous shunt may be an alternative rescue therapy for yellow nail syndrome.
- yellow nail syndrome
- chylothorax
- pleurovenous shunt
Statistics from Altmetric.com
Yellow nail syndrome is a rare disease consisting of a triad of conditions: yellow nails, lymphoedema, and pleural effusions that are sometimes chylous and massive.1–5 Massive pleural effusions and lymphoedema interfere with quality of life and can be life threatening because pleural effusions cause dyspnoea and chronic loss of chyle by serial thoracentesis leads to malnourishment. We present an elderly man who fulfilled the triad of yellow nail syndrome. To our knowledge this is the first report of a patient with yellow nail syndrome who was successfully treated with a pleurovenous shunt.
CASE REPORT
A 70 year old man was referred to Tenri Hospital with dyspnoea and leg oedema in July 2000. He noted that his nails were yellowish and had grown very slowly for 10 years before the referral. Oedema had developed in the left lower leg 5 years before the referral and gradually extended to both legs. He visited a nearby hospital in April 1999 and bilateral chylothorax was diagnosed. Diuretics were ineffective and he underwent repeated bilateral thoracentesis for relieving dyspnoea. More than 1.5 litres of chylous effusion was removed from each side once a month initially and twice a month just before the referral. There was no family history of lymphoedema.
Physical examination revealed decreased breath sounds at the base of both lungs. His body weight was 87 kg, height 174 cm, abdominal girth 105 cm, and right and left thigh circumferences were 51.1 and 55.0 cm, respectively. Marked oedema was present in the scrotum and lower extremities with thick and hyperkeratotic skin. The fingernails were thickened and had a yellowish hue, and onycholysis was present. Direct microscopic examination and culture of the nail clippings were negative for fungi.
A chest computed tomographic scan and magnetic resonance imaging revealed massive bilateral pleural effusions and normal bronchi, great vessels, and mediastinal structures. Thoracentesis yielded milky white fluid with a triglyceride content of 7.06 g/l on the right and 3.63 g/l on the left. The pleural effusions contained 300 white cells/mm3 with 47% lymphocytes, 0.5 mmol/l glucose and 14.7 IU/l adenosine deaminase on the right side and 500 white cells/mm3 with 53% lymphocytes, 0.55 mmol/l glucose and 11.6 IU/l adenosine deaminase on the left side. No malignant cells were found and cultures of fluids for bacteria and fungi were negative. Antifilarial antibody was negative in the serum. Radioisotope lymphoscintigraphy with technetium 99m-human serum albumin-diethylene triamine penta-acetic acid (99mTc-HSA-DTPA) revealed that lymphatic channels were grossly reduced in both legs. No activity was noted in the liver even 3 hours after injection. A diagnosis of yellow nail syndrome was made and open surgical pleurodesis was considered.
The patient preferred conservative treatment and was discharged from hospital. He continued to undergo serial bilateral thoracentesis at a nearby hospital. He returned to our hospital in March 2001 because thoracentesis every second week became inadequate for controlling the pleural effusions and his lymphoedema worsened. The levels of total protein and albumin in the serum were 44 and 21 g/l, respectively. Pleuroperitoneal drainage from the right pleural cavity to the peritoneal cavity was performed with a Denver-type shunt (Denver Biomaterials Inc, Golden, CO, USA) which consists of a peritoneal catheter, a pleural catheter, and a flexible 1.5 ml pump chamber containing a one-way mitre valve which is placed in the subcutaneous tissue, allowing manual compression to propel the fluid. He was instructed to compress the pump chamber 100 cycles four times per day. In the summer of 2001 he began to feel abdominal distension and stopped pumping the shunt. Although he underwent thoracentesis every second week at a nearby hospital, he had become bedridden and could not even roll over in his bed unassisted because of dyspnoea, severe fatigue, and massive oedema. He was readmitted to our hospital in December 2001.
His body weight was 109.5 kg, abdominal girth 127 cm, and thigh circumferences were 70 cm and 71 cm. The pleuroperitoneal shunt was replaced with a Denver-type pleurovenous shunt between the right pleural cavity and the right subclavian vein. Briefly, a pleural catheter was inserted from the sixth intercostal space under general anaesthesia. A subcutaneous pocket was created so that the pump chamber could be positioned over the lower rib cage. Flow of fluid was confirmed by compressing the pump chamber. The venous catheter was passed thorough a subcutaneous tunnel lateral to the breast and introduced into the right subclavian vein using the Seldinger technique. It was placed in the right side because chyle leakage may have occurred from the thoracic duct that runs on the same side in the thoracic cage. The extracted pleuroperitoneal shunt was patent. Dyspnoea, abdominal distension, lymphoedema, and daily activity gradually improved. One month after the implantation of the pleurovenous shunt the pleural effusions were well controlled (fig 1) and he could stand up unaided and sit in a wheelchair. His body weight decreased to 76 kg, his abdominal girth decreased to 97 cm, and right and left thigh circumferences decreased to 49 cm and 51 cm, respectively. The patient remained relatively healthy until 8 months after implantation of the pleurovenous shunt when he died suddenly at home of unknown causes.
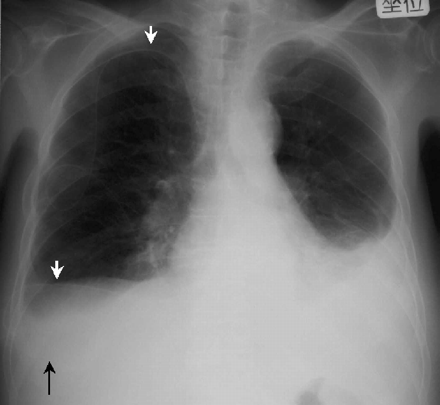
Chest radiograph 1 month after placement of a pleurovenous shunt between the right pleural cavity and right subclavian vein showing smaller pleural effusion on the right than on the left. The left pleural effusion did not increase without thoracentesis. The white arrows indicate a venous catheter and a pleural catheter and the black arrow indicates the site of a pump chamber which is invisible on the chest radiograph.
DISCUSSION
Yellow nail syndrome is a type of lymphatic dysplasia syndrome and hypoplastic lymphatic channels are observed with lymphangiography or lymphoscintigraphy in most patients.3 No specific treatment exists for this disorder and symptomatic treatment has been considered for dyspnoeic patients with massive pleural effusions.3,4 Medical management including medium chain triglyceride diet and diuretics is often inadequate, and surgical treatment is the only option for long term improvement.4 Open surgical pleurodesis or pleurectomy is recommended for low risk patients. Brofman et al5 found that a pleuroperitoneal shunt was effective for controlling pleural effusions in a patient with yellow nail syndrome. In our patient, however, a pleuroperitoneal shunt caused abdominal distension and worsening of lymphoedema, resulting in further deterioration in the quality of life. Implantation of a pleurovenous shunt has been reported in cases of malignant pleural effusion6 and in cases of hydrothorax with liver cirrhosis.7 In our patient a pleurovenous shunt was effective for controlling pleural effusions and lymphoedema. Moreover, the pleural effusion on both sides improved although the pleurovenous shunt was placed in the right side. Influx of chylous effusion into the left pleural cavity from the right side or from the abdominal cavity may have lessened, or leakage from thoracic lymphangiectasia may have decreased due to decompression of the lymphatic channel. Although the patient died suddenly of unknown causes, he had been able to enjoy a home life for 8 months. Implantation of a pleurovenous shunt may be an alternative rescue therapy for patients with yellow nail syndrome at high surgical risk when other conservative treatments have failed.