Article Text
Abstract
Background: A study was undertaken to evaluate whether adults differ from children in the indications and outcome of diaphragmatic plication following phrenic nerve injury.
Methods: A retrospective study was performed of 21 patients, 10 below the age of 5 and 11 older than 37 years. The indication for surgery for all the children was failure to wean from ventilatory support. The indications for surgery in the adult group were ventilator dependency (n=4) and symptomatic dyspnoea (n=7). All patients had at least one imaging study confirming diaphragmatic paralysis. The American Thoracic Society (ATS) dyspnoea scale, pulmonary function tests, and quantitative pulmonary perfusion scans were used as evaluation parameters. At surgery the diaphragm was centrally plicated.
Results: One child died immediately after surgery due to irreversible heart failure and two children died within 2 months of surgery from ongoing complications of their original condition. These three patients were considered as selection failures. Seven children were weaned from ventilatory support within a median of 4 days (range 2–140). Only one of four ventilated adults was successfully weaned. Seven adults who underwent surgery for chronic symptoms had a marked subjective improvement of 2–3 levels in the ATS dyspnoea scale. Pulmonary function studies in the seven symptomatic adults showed a 40% improvement above baseline. Severely asymmetrical perfusion scans reverted to a normal pattern after plication.
Conclusions: Diaphragmatic plication offers a significant benefit to children with diaphragmatic paralysis and should be performed early to facilitate weaning from mechanical ventilation. While plication is of limited benefit in weaning ventilated adults, it results in significant subjective and objective lifetime improvement in non-ventilated symptomatic adults.
- phrenic nerve paralysis
- diaphragm plication
- children
- pulmonary function tests
Statistics from Altmetric.com
Diaphragmatic paralysis (DP) following phrenic nerve injury is a well described entity which occurs in children and adults. It has clearly been shown that it is deleterious in children, especially in infants, often delaying or preventing weaning from mechanical ventilation. Because adult respiration is not as totally dependent on diaphragmatic breathing, DP is not as significant in them. It would appear that even when there is paralysis of the diaphragm, most adults can be weaned from ventilation.
Many reports have shown that unilateral diaphragmatic plication can reverse the ill effects of DP and facilitate early weaning in ventilated children.1–4 The role of diaphragmatic plication in adults with DP is not clear as only isolated case reports or small series of such patients have been reported.5–9
The present study was undertaken to compare the results in two distinct age groups and to determine whether plication has a similar role in adults as in children and infants.
METHODS
The records of all patients who underwent diaphragmatic plication at the Sheba Medical Center in Israel from 1988 to 2000 were reviewed. Surviving adults were interviewed individually. Preoperative and postoperative pulmonary function tests and quantitative pulmonary perfusion scans were performed in non-ventilated adults. Subjective dyspnoea was assessed by the American Thoracic Society (ATS) dyspnoea scale before and after surgery.
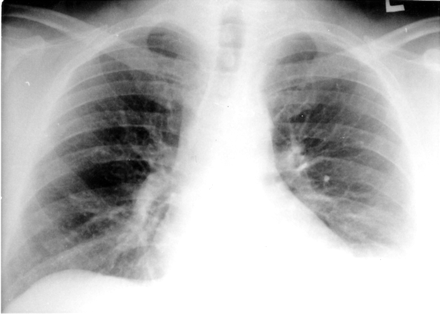
Twenty one patients were identified. The diagnosis of DP was established by chest radiography (fig 1) followed in all patients by fluoroscopy and/or ultrasonography and/or EMG stimulation. Nineteen patients underwent diaphragm plication through a posterolateral thoracotomy in the 6th intercostal space. Two neonates underwent plication via a mid line laparotomy. Video assisted procedures were not performed in this series. The diaphragm was plicated by a series of longitudinal U sutures placed in a posterior to anterior direction and reinforced at both ends over a Teflon buttress as described by Schwartz and Filler.1 In three adults the plication was reinforced by a Marlex mesh.
Chest radiograph 3 months after coronary artery bypass graft surgery showing markedly raised left hemidiaphragm.
RESULTS
Two groups of patients were defined. The first group comprised 10 children (table 1) aged 2 weeks to 5 years (mean and median 0.4 years). All cases in this age group were iatrogenic following surgery mainly for a congenital heart condition (n=9) and all suffered from an inability to wean from mechanical ventilation. Seven children had right sided and three had left sided paralysis. The duration of mechanical ventilation before plication was 11–152 days (median 35 days) and the interval from plication until extubation was 2–140 days (median 4 days). In six children early extubation (2–8 days) was possible. There were no further respiratory problems and all were discharged in good condition following extubation. One infant died within 2 hours of a combined cardiac operation and diaphragm plication due to intractable heart failure. Two children died from complications of pneumonia and congestive heart failure due primarily to their underlying heart condition, despite a radiologically successful plication.
Summary of the paediatric group
The second group comprised 11 adults aged 37–76 years (mean 65) with DP mainly related to previous cardiovascular surgery. Despite DP, seven of these adults were weaned from ventilation within 24 hours of the causative surgery. Four (table 2) were mechanically ventilated at the time of plication. Following plication one was extubated within 2 days; the other three ventilated patients did not benefit from the plication. One was transferred ventilated to his home country after 35 days and two succumbed from complications of their underlying disease.
Results in ventilated adults
The other seven adults (table 3) suffered from varying degrees of progressive dyspnoea scored according to the ATS dyspnoea scale. None of them had a history of chronic respiratory disease. All had a complete work up which ruled out a cardiac reason for their severe dyspnoea. Preoperative lung function tests (table 4) showed a restrictive pattern and a quantitative pulmonary perfusion scan showed a marked reduction in flow on the affected side (mean 32%).
Results in non-ventilated adults
Pulmonary function tests for symptomatic adults
Following plication all of the adult survivors described improved ATS dyspnoea scores of 2 (n=3) or 3 (n=4) levels. Chest radiographs showed the return of the diaphragm to a normal position (fig 2). Postoperative total lung capacity (TLC), forced vital capacity (FVC), and forced expiratory volume in 1 second (FEV1) improved above baseline preoperative measurements in all patients (31–71%, 23–66%, and 29–47%, respectively). Perfusion scans returned essentially to normal after surgery from a mean of 32% perfusion on the affected side to 45%. The youngest patient in this group (age 37, aetiology trauma) suffered from moderate dyspnoea at rest. His major complaint was severe restricting dyspnoea during sexual activity. Following plication he has had no dyspnoea and enjoys a normal sex life. Three asymptomatic patients died many months after their plication from conditions unrelated to DP. The four surviving patients (mean follow up 88 months) are all asymptomatic.
Chest radiograph 3 weeks after diaphragmatic plication showing the left hemidiaphragm in a normal position.
DISCUSSION
Phrenic nerve injury causes diaphragm muscle dysfunction which results in impaired work and efficiency of breathing. Paralysis of the diaphragm may produce severe respiratory difficulties due to the paradoxical motion of the affected diaphragm and a similar shift of the mobile mediastinum. Tachypnoea, atelectasis, pneumonia, and continued respiratory distress and CO2 retention may develop after extubation. Diaphragmatic dysfunction can result in inability of the patient to be weaned from mechanical ventilation after surgery.
Paralysis of the diaphragm usually occurs after trauma to the phrenic nerve. In children the most common aetiologies are birth trauma10–13 and congenital diaphragmatic eventration.14 The incidence of unilateral phrenic nerve paralysis following paediatric heart surgery has been reported in different series to vary from 0.46% to 4.6%, with the highest incidence after a Blalock-Taussig shunt.15
In all age groups DP has been reported with increasing frequency after open heart surgery16–21 and is mainly related to topical cooling.22 In adults DP has also been reported after external trauma23 or as a result of tumour growth.
The diagnosis of DP is suggested when the chest radiograph shows a raised diaphragm and is confirmed by oesophageal and gastric pressure measurements,24 fluoroscopy, ultrasonography and, most definitively, by EMG stimulation. The sniff test confers no advantage over ultrasonography which should be considered the diagnostic method of choice.25
The younger the patient, the more serious the consequences of unilateral phrenic paralysis. Children older than 2 years tolerate DP better and can be extubated early without plication. Adults tolerate DP and are generally able to compensate for the inefficient mechanical respiratory function. Many studies have shown that most cases of phrenic nerve paralysis following cardiac surgery are transient and of no clinical significance. However, some adults require continued mechanical ventilation and in these DP is only one factor contributing to their postoperative pulmonary insufficiency. Ipsilateral pneumonia may persist and interfere with weaning. Other adults may be successfully weaned from the ventilator but remain severely limited in activity.
Diaphragmatic plication is intended to decrease lung compression, stabilise the thoracic cage and mediastinum, and strengthen the respiratory action of intercostal and abdominal muscles. More effective diaphragmatic recruitment occurs after plication leading to increased diaphragmatic strength and maximal voluntary ventilation. Studies have shown objective evidence that all lung volumes with the exception of FRC are improved following plication.6–8,26,27 The beneficial effect of diaphragmatic plication has been shown to be long lasting and does not interfere with return of diaphragmatic function which may occur spontaneously within 18 months, but may take as long as 3 years. In children the plicated diaphragm maintains its growth in proportion to the other side.28
While some studies20,29 have shown that recovery occurs spontaneously in 90% of children, a mean time of 40.8 days until extubation is required. A consensus has therefore evolved that children with DP who cannot be weaned after 2 weeks of mechanical ventilation should undergo plication.
The results in our group of 10 children confirm the benefit of early plication. Six patients were extubated within 2–8 days (mean 3.5). Plication was performed in the first patient after 130 days of mechanical ventilation. By that time the patient was so septic that plication provided little benefit in accelerating extubation. Three patients succumbed to the severe haemodynamic complications of their congenital heart disease. A better selection of patients could have prevented these unnecessary operations. The interval to plication in our series was too long. In the first three cases we had a learning curve and had to convince the primary care physicians as to the efficacy of the procedure. Later in our experience the interval was shortened but has not yet reached the optimal period of 2 weeks.
The group of 11 adult patients shows a clear difference from the paediatric group. As anticipated, most adults with DP could be weaned from ventilation without plication. Four mechanically ventilated adults were plicated and only one of them was weaned. The other three continued to be ventilated for an extended period until they succumbed to the progression of their underlying conditions and resulting complications. Retrospectively, plication was probably not indicated in these patients because all three had severe pulmonary parenchymal disease at the time of plication.
The results in adults with progressive and debilitating dyspnoea were excellent. There was no operative mortality or morbidity, hospitalisation was short, and the results were highly satisfactory in all cases. All had a decrease in breathlessness as measured by the ATS dyspnoea scale and an improved quality of life and satisfaction with their operation.
The improvement in pulmonary function over baseline measurements was considerable. Even more impressive was the major improvement in lung perfusion scans. In all cases the quantitative perfusion scan returned almost to normal, indicating that the entire improvement in pulmonary function indeed resulted from increased ventilation and perfusion on the operated side. The combined results of pulmonary function tests and perfusion scans indicate that the paralysed side was responsible for the respiratory complaints.
We conclude that early diaphragmatic plication in properly selected ventilated infants with DP offers immediate benefits and excellent results and prevents the complications of prolonged mechanical ventilation. A policy of early diagnosis of DP and early treatment using plication in children with failure to wean should be adopted. Infants with severe cardiomyopathy and progressive pulmonary parenchymal damage should be denied surgery.
In adults, plication is rarely indicated as a means of accelerating weaning from mechanical ventilation. However, adults with chronic symptoms can benefit significantly from plication. Combined pulmonary function tests and quantitative perfusion scans are helpful in selecting patients for this procedure.